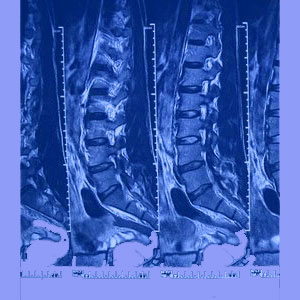
Sciatica MRI is an advanced diagnostic imaging tool which completely visualizes the entire diversity of spinal structures in an effort to determine the exact anatomical source of symptoms. Magnetic resonance imaging is perhaps the best tool a back, neck or sciatica pain specialist can use to determine what is going on inside the vertebral column to create such agonizingly painful syndromes.
However, the MRI is limited to helping to diagnose some varieties of structural pain conditions and often creates the perfect circumstances for misdiagnosed sciatica syndromes in patients with circumstantial spinal abnormalities which may be used as bogus evidence supporting a misdiagnosed causative conclusion. In essence, although the test is highly detailed and accurate, it is still subject to interpretation, making it just another tool which is abused by some less ethical and economically motivated caregivers. This is a basic fact which all patients must understand before speaking to any doctor about the results of their sciatica MRI evaluation.
This article will provide the pros and cons of using MRI to help identify the true cause of pain in sciatica patients.
What is a Sciatica MRI?
Patients with long-term or serious potentially spinally-motivated pain should always undergo a CT scan or better yet, an MRI. The test will show the vertebral bones and intervertebral discs in amazing detail and clarity.
Degenerative disc disease is easily diagnosed using an MRI, as are herniated discs. Other common processes often blamed for back pain, such as facet joint degeneration and osteoarthritis can also be imaged, as well as their potential effects on surrounding spinal nerve roots.
MRI will make diagnosis of obvious conditions very easy, but might also create a world of confusion when a spinal abnormality exists coincidentally in the general area of the painful complaint. In these cases, the causation of pain is typically blamed on the scapegoat condition, even if there is considerable doubt as to whether or not that abnormality is actually to blame for anything at all. This is one of the main justifications for the gross misdiagnosis of many sciatica conditions.
MRI Interpretation
The role played by the radiologist is crucial when it comes to reading an MRI. Give the same films to 5 different radiologists and you are likely to get 5 very different reports. The problem with sciatica MRI is that it is subject to a great amount of speculation and interpretation.
Doctors can play up or play down any number of possible causes of pain and often choose the former option when it comes time to make some money. For example, I had 2 MRI tests done, one in my middle 20’s and one a few years later. Both sets of films were passed around to a great number of doctors who read them and interpreted the results. I received a variety of diagnoses and many doctors disagreed on the actual source of pain.
Sure, they all saw 2 herniations, but some saw other things and some did not. Some placed the blame for the pain directly on the herniated discs, while others realized that the actual symptoms did not exactly correlate to the clinical diagnosis.
Sciatica MRI Experiences
I learned a whole lot more about how MRI films are speculated upon from Dr. John Sarno, who did not seem to care one bit about anything he saw on my MRI films. Herniated discs? So what. Degenerative disc disease? That’s no disease. That’s normal. This was Dr. Sarno’s opinion. It turned out to be the most enlightened of all.
For years, the wonderful images produced by those miraculous MRI devices clearly showed what seemed to be the perfectly logical reason for my pain. What the films did not show was far more important. The images did not reflect the 10 other herniations in my neck and upper back, not discovered until many years later. Therefore, they did not show the serious spinal cord displacement and other problems enacted by these disc pathologies.
Furthermore, the MRI did not take into account the stress I suffered and how this mindbody component influenced my pain. These were clearly serious limitations to its usefulness in my own case at this stage of my back and neck pain nightmare.
MRI is a great tool, but is also a huge contributor to the diagnostic nocebo effect which is so damaging to the patient. In fact, the nocebo is sometimes far more injurious than any suspected physical source of back pain could ever be. Nocebo takes your health away and eventually might take your very life.
Sciatica Magnetic Resonance Imaging
So, the bottom line comes down to this: Sure, get an MRI. In fact, get several. Image the whole spine, if possible. Use these tools to help you to find the reason for your pain. However, be aware of the limitations and even drawbacks of MRI.
First, the interpretation of the images is a highly subjective process. Just because a spinal abnormality is seen, does not mean that it is in any way responsible for your pain.
Second, MRI does not replace neurological testing or symptom correlation. These are crucial aspects of achieving an accurate diagnosis.
Finally, in some instances, a sciatica MRI study can be a propaganda tool which is literally used to enslave patients into unneeded and even contraindicated treatment of some spinal irregularity which demonstrates no pathological process at all. In fact, this is the exact reason why so many patients undergo completely unnecessary sciatica surgeries.





