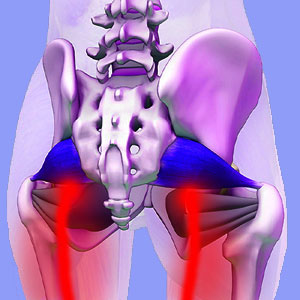
Having the sciatic nerve compressed by piriformis muscle can cause chronic pseudo-sciatica symptoms often diagnosed as piriformis syndrome. The pain can be terrible and might limit physical functionality to a large degree. Additional symptoms might often include tingling, numbness and weakness in various parts of the lower limbs, unilaterally or bilaterally.
Piriformis syndrome remains a controversial diagnosis, but we can assure you that the condition does exist. However, it is diagnosed more often than it actually occurs, especially when the diagnosis is one of revision following an initial diagnosis of lumbar pathology.
This essay explores how and why the piriformis muscle might interact negatively with the sciatic nerve. If you are a patient who suspects piriformis syndrome is the root cause of your suffering, or a patient who has been formally diagnosed with piriformis syndrome, then this is the perfect dialog for you.
How is the Sciatic Nerve Compressed by the Piriformis Muscle?
Some people are born with a congenital abnormality of the sciatic nerve pathway. This can place the nerve in abnormal proximity to the piriformis muscle or even position it through the substance of the muscle. It should be known that a significant percentage of people who receive a diagnosis of piriformis syndrome demonstrate these atypical sciatic nerve locations.
In other cases, no abnormality exists, yet the piriformis spasms and constricts the sciatic nerve even though it remains in its textbook typical position.
Compression of the sciatic nerve can take many forms, from a single acute episode to recurring flare-ups to chronic and unrelenting impingement. Therefore, although the symptoms might be similar initially, the eventual expressions of piriformis syndrome can be very different from one patient to another. This is because flare-ups tend to favor pain as a primary expression that might come and go, while chronic compression might cause numbness and weakness in the muscles of the legs and/or feet due to a lack of proper innervation. In some cases, dysfunction might result, as well, such as the expression of dorsiflexion deficit, also known as foot drop.
Piriformis Sciatica Controversy
The piriformis syndrome diagnosis remains controversial for many justifiable reasons, including all of the following facts:
Many people who demonstrate sciatic nerve abnormalities, such as the nerve running through the muscle, never develop pain.
Many people with sciatica might be categorized into the piriformis syndrome diagnosis simply because they demonstrate nerve-through-muscle abnormalities, even if there is no evidence of compression within the muscle. In essence, the anatomical atypicality might be incidental, but acts as a common scapegoat to explain symptoms.
In cases where no anatomical abnormality exists, symptoms can also exist and be just as fierce as in people with sciatic nerve positional irregularities.
Although symptoms are virtually always blamed on piriformis spasms, few care providers can explain why the muscle is spasming. What is the root process causing the muscle to clamp down on the nerve? This is an excellent question, especially since most diagnosed patients have no history of injury to the region.
Sciatic Nerve Compressed by Piriformis Muscle Relief
We have seen some cases of piriformis syndrome that were exactly as medical science describes them… perfect examples of the sciatic nerve compressed by the piriformis muscle due to anatomical atypicality, history of piriformis injury, obvious piriformis imbalance or other structural causation.
However, in most cases of piriformis syndrome, there is no explanation for why the muscle is in spasm. In our experience, the root causative process is virtually always ischemia. We know this to be true, since treating the ischemia resolves the pain almost universally.
We also see many cases of misdiagnosed piriformis syndrome. In rare cases, the pain might actually be true spinally-motivated sciatica. In other cases, there might be another cause locally or systemically to explain the symptomology. However, once again, the majority of cases we see tend to be caused by regional ischemia that targets the sciatic nerve roots in the lower spine, as well as the postural muscles and sometimes, even the piriformis muscle, as well. Once again we know this to be factual, since treating the root source of oxygen deprivation brings relief almost universally.
Sciatica > Sciatica Diagnosis > Sciatic Nerve Compressed by Piriformis Muscle





