Sciatica from a pinched nerve is the most common diagnosis used to explain typical lower back and leg pain conditions. The usual diagnostic model theorizes that one of the spinal nerve roots in the lumbar region is being impinged upon, most often by a herniated disc or osteoarthritic bone spur complex. While this can and does occur in some rare instances, the incidence of misdiagnosis is high, leading to the abysmal curative statistics for attempted therapies. Of all suspected sources of sciatica, nerve compression conditions are some of the most difficult to accurately and correctly diagnose.
This essay covers the incidence of sciatica caused by compressive neuropathy issues in the lower spinal regions. We will detail pinched nerves and how they may cause symptoms in areas far away from the actual compression.
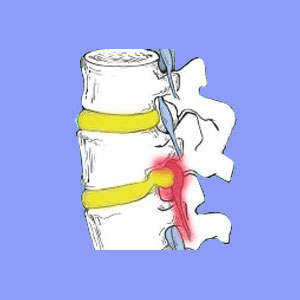
Sciatica from a Pinched Nerve / Foraminal
It is entirely possible for an osteophyte complex or a herniated disc to completely block the neuroforaminal space, leading to compression of a nerve root. However, this event is very rare. Far more often, mild narrowing of the neuroforamen and suspected, but not verified, impingement of a nerve structure leads to a definitive diagnosis of compressive neuropathy. This is a terribly problematic concern.
In most cases, the spinal nerve is not being affected at all, or at least not to the extent of explaining the symptoms. This is also why treatments designed to cure pinched nerve fail so often. In essence, the narrowed foraminal space is nothing more than a coincidence to the pain. Research has shown that virtually every person suffers reduced neuroforamen, since this is normal during the aging process, but we do not all have pain, and even those who do, might have pain at a location which is structurally healthier than a completely degenerated, yet totally asymptomatic area. This is illogical following the purely structural model of sciatica.
As previously mentioned, a completely closed off foraminal space can enact symptoms. However, these symptoms have been laboriously studied in the laboratory and consist mostly of eventual objective numbness and subsequent weakness. This describes a total lack of nerve sensation. This is not pain, not tingling and certainly not the subjective numbness common to most sciatica sufferers. These subjective symptoms do not make sense from a chronically pinched nerve.
Sciatica from Central Canal Stenosis
In the lower back, the spinal cord has already branched off to become the cauda equina. The actual cord ends in the uppermost lumbar spine, but the nerve roots continue to traverse the central spinal canal, massed together, until they each exit through their respective neuroforaminal openings.
Being that these nerve roots can now be affected within the central canal, spinal stenosis may elicit symptoms of a pinched nerve, even though the compression occurs centrally and not foraminally. Any variety of stenotic change to the central canal can cause one or more of the nerve roots to induce symptoms locally and in the anatomical areas served by the impinged tissue.
Since some spinal stenosis concerns affect multiple nerve roots, sciatica might be far more of a logical conclusion, especially in patients whose symptoms are wide ranging and variable.
Observations of Sciatica from a Pinched Nerve
Verified nerve compression syndromes are not subject to debate. There is obvious dysfunction of sensory and motor function, as well as a host of other problematic effects, including cauda equina syndrome. These events do occur.
Actual pinched nerve sciatica complaints do do not represent the average sciatica sufferer who has been misled into believing that a minor herniated disc at L4/L5 or L5/S1 is causing all their pain. They do not represent that person with spinal osteoarthritis whose pain has been blamed on a narrowed, but still functional neuroforaminal opening. They certainly do not represent the person whose diagnosis has been revised 6 times over the course of 20 years in an effort to cover up diagnostic incompetence.
Be warned, pinched nerves will respond to correct treatment. If your compressive neuropathy does not, consider diagnostic error as the most logical explanation and consider seeking out an alternative explanation for your pain by getting a second opinion. You can also learn the real facts about pinched nerves from Cure-Back-Pain.Org. Their pinched nerve resource section is the best on the web.





