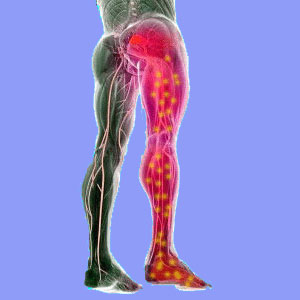
Sciatica pins and needles is a colloquial term for the tingling and numbness often associated with this epidemic lower back and leg pain syndrome. Pins and needles can be experienced anywhere in the lower body with a sciatic nerve pain condition, but are most common in the buttocks, entire leg, rear thigh, side thigh, rear calf, side calf and feet.
This article will expound on previous site offerings related to paresthesia in the buttocks, legs and/or feet. We will discuss many lesser known concepts about why tingling can occur in the lower limbs and how it may be mistakenly linked to innocent lumbar spinal issues.
Pins and Needles Defined
Chronic pins and needles are statistically most often the result of either a nerve compression syndrome in the spine or an oxygen deprivation syndrome, typically enacted by a psychosomatic sciatica source.
Pinched nerves due to foraminal stenosis are a very common diagnosis, often linked to herniated discs and arthritic osteophytes. However, these conditions are often misdiagnosed, since the disc or bone spur material would have to virtually completely block the neuroforaminal space in order to truly enact significant neurological issues. This rarely is the case in most diagnosed patients. Since the cauda equina has already replaced the spinal cord in the mid to lower lumbar area, it is certainly possible for pinched nerves to occur within the central canal or lateral recesses, as well.
Nerve conduction testing and subsequent correlation of neurological effects can help sort out true lumbar compressive neuropathy issues from innocent and incidental stenotic change.
Ischemia is seldom diagnosed, since medical doctors are simply not trained to recognize the signs of this rampant emotionally-induced condition. Luckily, knowledge therapy is a good solution for chronic sciatica due to ischemia, since there is no risk and no expense whatsoever. In cases where ischemia is driven by a purely physical process, such as a systemic or localized vascular tissue disorder, the process is usually discovered early in the diagnostic process by any thorough neurologist.
Sciatica Pins and Needles Explanations
Pins and needles may come on with particular activities or positions. This is sometimes possible with bone spurs and herniations impinging on nerve roots, but is far more usual with ischemia.
For patients who experience structurally-illogical symptoms, such as many night time sciatica conditions, the true source may turn out to be oxygen deprivation, no matter how the condition was originally diagnosed.
It is crucial to remember that actual complete compression of a spinal nerve root will cause that nerve to stop signaling altogether. The result is true numbness, not tingling or the subjective numbness common in most sciatica sufferers.
Pins and needles might be caused by a partially compressed nerve root, although this can be a highly speculative diagnostic theory.
In many cases, however, widespread tingling can certainly be caused by central spinal stenosis in the upper regions of the vertebral column. This is another one of the structural issues which typically eludes proper diagnosis, since professional focus is usually limited to the lumbar region, which is most often chock full of scapegoat abnormalities just waiting to be misdiagnosed as the underlying reason for the symptomatic expression. I see this all the time.
Sciatica Pins and Needles Conclusions
Sciatica is known to be a misery, as well as an incredibly difficult to cure condition. There is no definitive anatomical reason for the pain in most instances and even when a structural source is targeted, the diagnosis is often ill conceived.
Most of the structural issues blamed for causing sciatica have never been clearly defined with any pathological component or process. Sure, you might have arthritis or a herniated disc, but if these irregularities are not influencing a nerve, then they are typically circumstantial and not causative. This is medical fact.
If the diagnosis is wrong, then the treatment selected will also be wrong. This is a much more sensible explanation than stating that the dozens of sciatica treatment options you may have tried all failed for some unknown reason. Of course they failed, the diagnosis is probably incorrect.
In summary, it is worth noting that correct diagnosis with verified evidence of a nerve compression scenario typically does resolve with appropriate care. When this fails to occur, now at least now you will have some clue as to why.





