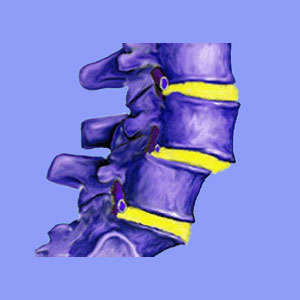
Spondylolisthesis is a spinal abnormality which most commonly affects the L4 or L5 vertebrae. The condition is characterized by slippage of the affected vertebra, in relation to the rest of the spinal column. Anterolisthesis is defined as a forward slippage, while retrolisthesis is a rearward vertebral migration. Although the condition is not unusual and rarely causes any pain in its milder forms, it might be responsible for creating symptoms in a minority of patients and is certainly used as a sciatica scapegoat to explain pain in others.
This dialog will investigate the diagnosis of vertebral slippage in the lumbar spine and provide insight how this structural irregularity might cause or contribute to sciatica through nerve root impingement. We will also explore the full range of possible vertebral migration severities and how the grade of the condition is usually indicative of its symptomatic effects.
Spondylolisthesis Conditions
Vertebral slippage can occur from injury, osteoarthritis, genetic influence or idiopathic reasons. Slippage is measured by percentage, rather than by an exact measurement, since every spine has different dimensions. Measuring the condition using the percentage of overlap which occurs between the normal vertebrae and the affected vertebra is the best way of getting an objective and relative view of the extent of the potential problem. Typically, the scale is rated as:
Grade 1 = less than 25% slippage.
Grade 2 = more than 25% but less than 50% slippage.
Grade 3 = more than 50% but less than 75% slippage.
Grade 4 = more than 75% but less than 100% slippage.
Grade 5 = more than 100% slippage (also called spondyloptosis).
Grade 1 and 2 conditions are the most commonly reported asymptomatic forms, although some cases can still create problems in select patients. However, to provide a balanced view, pain is not inherent to even severe cases of vertebral misalignment and some grade 3 patients are still asymptomatic. You can get a complete view of spondylolisthesis from the best website devoted to the topic of vertebral migration. Check out Spondylolisthesis-Pain.Com for everything related to vertebral slippage.
Vertebral Misalignment Symptoms
Most minor vertebral slippages are not symptomatic or functionally limiting in any way. These account for most grade 1 and 2 conditions and are often not even discovered until much later in life.
Beginning at grade 3, the percentage of patients who might suffer problematic symptoms increases steadily. Obviously, with larger degrees of vertebral slippage, there are also increased risks for pain, neurological symptoms and spinal instability. Luckily, most diagnosed conditions are low grade and will not require any specialized care or concern.
When symptoms do occur, it is usually for one of two possible reasons. Minor localized pain may be related to mechanical interactions between misaligned bones. Widespread, radiating pain and related neurological expressions might indicate nerve involvement. This usually means that one or more nerve roots are being compressed, either within the central canal or as they try to exit through unaligned foraminal openings.
Read more about sciatica from spondylolisthesis.
Spondylolisthesis Help
Accurate diagnosis is crucial with this condition, just like all dorsopathy syndromes. If you see vertebral slippage on an x-ray, it can look very scary and might create quite a nocebo effect, even if the condition is inherently harmless.
The way the diagnosis is presented to the patient will also contribute greatly to the likelihood of possible symptoms in the future. If the patient is frightened, symptoms are likely, but if the patient is reassured, grade 1 and 2 slippages are statistically unlikely to cause any significant chronic pain.
Minor versions of vertebral misalignment are used as a sciatica scapegoat in many patients who demonstrate even the slightest amount of slippage due to completely normal osteoarthritic processes. This type of vertebral movement usually occurs after middle age and is virtually never the cause of pain.
If you have been diagnosed with vertebral slippage, make sure to get a very detailed diagnosis including the degree of slippage and the stability of the spine. This is crucial in deciding whether this is a real concern or just another harmless abnormality which is unfairly blamed for sciatica pain.





