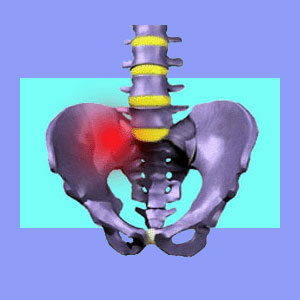
Sacroiliac pain is a controversial diagnosis which has grown in prevalence in the last 2 decades. This condition can resemble some varieties of sciatica in its symptoms, including pain, tingling and numbness in parts of the lower body, including the buttocks, pelvis and even upper legs. However, sacroiliac discomfort it is a distinctly different disorder.
This article details the similarities and differences between sciatica and sacroiliac joint symptoms. We will discus how SI joint concerns are sometimes mistakenly theorized to cause illogical sciatica expressions, as well as how sacroiliac pain may be mistakenly linked to any of the usual lumbar spinal abnormalities.
Sacroiliac Pain Explained
The sacroiliac joint is one of the strongest in the human body. It must bear the weight of the entire upper body at the junctures of the sacrum and the pelvic ilium. The joint is surrounded by the sacroiliac ligaments which are tough as nails. There are 2 common varieties of true sacroiliac symptoms:
Osteoarthritis can cause degenerative changes in the bones, just like anywhere else in the body. This condition is sometimes called sacroiliitis.
Sacroiliac joint dysfunction is often diagnosed when there is a suspected problem with the ligaments which encapsulate the joint. Typically, the ligaments are too loose, which provides abnormal joint movement, although sometimes they can be too tight, causing an overall reduction of movement.
The expressions of either condition are usually expressed locally, deeply in the buttocks or pelvis. Symptoms may be unilateral or bilateral, affecting one side or both.
Sacroiliac joint pain is profiled in complete detail on our partner web property The Sacroiliac Authority. We suggest reading this resource for more information on how the SIJ can cause sciatica symptoms.
Sacroiliac Joint Causing Pseudo-Sciatica
This condition is one of several which can be described as pseudo-sciatica pain syndromes. The name comes from the fact that although the symptoms may mimic spinally-induced sciatic nerve pain, the source is not directly related to spinal nerve compression. The other commonly diagnosed variety of pseudo-sciatica is piriformis syndrome.
Sciatica from sacroiliac diagnoses are usually accomplished through the process of elimination, hence their controversial nature. It is very difficult to prove that a sacroiliac joint abnormality exists, but it is virtually impossible to disprove it. This is because soft tissue concerns affecting the ligaments are difficult to image or verify, while actual joint deterioration is normal to some degree, making it seen in virtually everyone.
If sciatica exists and the doctor can not find a convincing reason for it in the spine, then the diagnostic process will typically widen and might focus on the sacroiliac region and the piriformis muscle.
When it comes to piriformis syndrome and sacroiliac joint problems, the anatomical structures are so close in location and the symptoms can be so similar, that they are sometimes misidentified interchangeably in the diagnostic process. Know that piriformis syndrome is likely to enact symptoms which mirror true sciatica in a diversity of locations and expressions. SI joint pain is more likely to be localized and lack neurological components, like numbness or tingling, although these are not absolute rules.
Sacroiliac Pain Overview
Personally, I share the view expressed by many medical professionals. A good number of doctors see sacroiliac concerns as some of the latest diagnoses which are often made by exclusion and are typically incorrect.
Be very careful carrying around the significant burden of a SI joint diagnosis. You must understand that the SI joint is ridiculously strong and resistant to degeneration. Even when a pathological condition does exist, it is not likely to cause the type of far radiating pain normally seen with true sciatica.
Keep these factors in mind if your doctor or chiropractor begins blaming your SI joint after other diagnostic theories have proven incorrect. This one will most often follow suit, leading to more failed treatments.





