Piriformis pain, commonly referred to as piriformis syndrome, is another of the pseudo-sciatica diagnoses used to explain symptoms which appear to be sciatica pain, but are not caused by a spinal nerve compression condition. Piriformis syndrome is a very real condition, but like many other sciatica scapegoats, is diagnosed far more often than it actually occurs. We have seen an increase in the rate of diagnosis of piriformis syndrome over the past decade, as well as a dramatic increase in the number of misdiagnosed cases.
This article will explain piriformis-induced symptoms and how this powerful muscle may be responsible for causing chronic sciatic nerve pain.
What is Piriformis Pain?
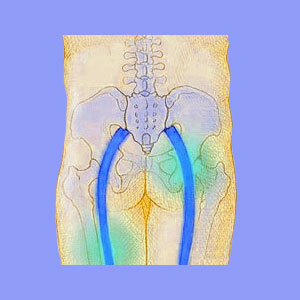
Piriformis syndrome describes a condition where the sciatic nerve is constricted or impinged upon by the piriformis muscle, as it exits the greater sciatic foramen. This muscle usually rests on top of the sciatic nerve, but in some people, actually surrounds the nerve.
It is theorized that patients with piriformis syndrome are experiencing sciatica symptoms due to the piriformis muscle squeezing the sciatic nerve due to trauma or ischemia. The muscle goes into chronic spasm, clamping down on the nerve and eliciting symtoms.
Piriformis syndrome is typically identified through physical exam and the process of elimination, very much like sacroiliac pain. Final diagnosis is often made by anesthetic injection, which is known to be a faulty and far from accurate diagnostic practice. Read more about sciatica from piriformis syndrome.
Piriformis Syndrome Condition
While piriformis syndrome is more prevalent amongst patients who do have the physical abnormality of a piriformis muscle surrounding the sciatic nerve, it is still highly controversial. Most cases of nerve constriction are based on trauma to the piriformis and in many cases; there has been no trauma, nor signs of any trauma. It is idiopathic why the piriformis would suddenly begin to constrict the sciatic nerve in most diagnosed patients.
Ischemia can target this muscle as part of a regional oxygen deprivation syndrome explaining the constriction far more logically.
However, treating the piriformis itself in these cases is poor medicine and ineffective symptomatic therapy. It is instead advised to deal with the underlying psychoemotional cause of the ischemia to seek symptomatic resolution and this usually involves treatment using knowledge therapy.
Piriformis Pain Analysis
I have received a steadily increasing supply of letters from patients who have been diagnosed with this painful condition. It certainly exists, but why it creates symptoms is the basis of my concern. The idea that some form of degeneration or trauma has injured the piriformis is generally completely incorrect and baseless. The incidence of ischemia acting on the piriformis seems very plausible.
As with all ischemic sciatica situations, I often refer the patient to knowledge therapy as the best approach to sciatica treatment. There are no risks and no expenses, so there is nothing to lose, except the pain and the incorrect diagnosis. If you need to know more about piriformis pain, then you must read the research on The Piriformis Authority web resource for complete coverage.




