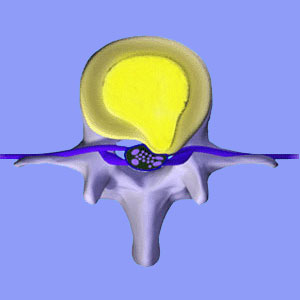
Suffering permanent sciatic nerve damage from a herniated disc is part of many patient worries, since lots of lower back pain sufferers have been told that a compromised intervertebral disc can injure this vital neurological structure. Unfortunately, most of these patients do not truly understand the details of their lumbar anatomy and probably do not even know that the sciatic nerve never attaches directly to the spine. Therefore, they do not comprehend that injury to the sciatic nerve is not even possible from any disc pathology.
The goal of this article is to dispel the myths concerning sciatic nerve injury and herniated discs, as well as enlighten patients as to what is actually going on when they have a lumbar or lumbosacral herniation in their spine that produces sciatica symptoms.
Real Sciatic Nerve Damage from a Herniated Disc
Is sciatic nerve injury even possible from a bulging disc? …and the answer, technically, is a definitive no. This is because the sciatic nerve never joins the spinal column directly, so there is a zero percent chance that a herniation will damage the nerve itself.
What can happen, in extreme instances, is that one or more of the spinal nerve roots which eventually go on to form the sciatic nerve may be injured or compressed by the herniation. This is possible, but is a subject of unwarranted fear in many circumstances.
Just for the record, nerve damage means a temporary or permanent reduction in the normal functionality of the affected nerve structure. This is not an inherently painful condition, and in many cases, the actual damage inflicted will prevent any pain from ever occurring, since the nerve is not signaling at all.
Remember, countless proven research studies have shown that continuing compression of any neurological structure will cause that nerve to stop functioning. This results in paresthesia, not the chronic pain most often associated with sciatica.
Sciatic Nerve Injury from a Bulging Disc
The sciatic nerve is made up of the pairs of bilateral spinal nerve roots at L4, L5, S1, S2 and S3. It is the largest nerve in the body and runs down each leg, forming the network of peripheral nerves which serve the neurological needs of almost the entire lower anatomy.
Herniated discs can encroach upon, touch and even impinge on one or more spinal nerves without causing any pain or symptoms whatsoever. It is only when the nerve is truly compressed that symptoms will almost surely ensue. In these cases, the symptoms may be painful for a short time, but will usually lead to objective numbness and weakness in the affected areas served. Most of these cases can be successfully resolved using appropriate invasive or noninvasive therapies without suffering lasting damage to the nerve from the disc herniation itself.
It should be noted that in a great number of cases where postoperative patients suffer nerve injury, the damage is not from the herniation, but instead caused directly by the herniated disc surgery used to treat the condition. In many cases, the operation has definitely caused more harm than good, explaining why I am generally so anti-surgery in my outlook for treatment.
Sciatic Nerve Damage from a Herniated Disc Facts
Most herniations will do no harm to the spinal nerves. In fact, the overwhelming majority of intervertebral bulges, protrusions and ruptures are innocent of causing any health problems at all. Some pathological disc conditions can enact structural changes which may cause symptoms and some will enact structural changes which will definitively cause symptomatic expression.
Very few bulging discs will cause permanent nerve damage, unless the force of the herniation is extreme or the protrusion calcifies and slowly wears away at the nerve like a saw.
In some scenarios where patients write to us fearing paralysis, nerve damage or complete disability from minor and normal disc issues, it is obvious that these poor souls are being used and abused by greedy and doctors and/or chiropractors who see an easy mark and an easier payday. The diagnostic evidence of their conditions rarely supports any symptomatic expression at all; forget about any such terrifying conclusions which fill their minds with fear.
It is a real shame that our healthcare system has come to this. However, there are still many good doctors who can set you on the right path and clarify your condition, assuaging your fears in the process. If you have been terrified by your doctor, this is probably a good indication of one of 2 possibilities:
You are actually in really bad shape, but your doctor’s bedside manner needs some drastic improvement. Doctors must be careful of the language they use and the threats they imply to any patient’s health.
The psychoemotional impact of these tactics can be far worse than any structural issue could ever be. Consider getting at least a second, and possibly a third, opinion before acting on any treatment recommendation.
You might be on the wrong path altogether and should think about finding a new doctor, unless your goal in life is to suffer endlessly in order to pay for your doctor’s exorbitant and luxurious lifestyle. This is particularly true if another diagnostician have already provided contrasting evidence that the disc may not be causative.
Sciatica > Sciatica Advice > Sciatic Nerve Damage from a Herniated Disc





