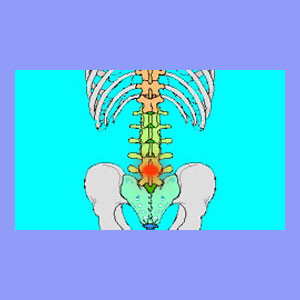
Sciatica L5 is a specific diagnostic conclusion relating to impingement of the lumbar 5 spinal nerve root.
L5 is one of the nerves which join together to form the sciatic nerve. L5 is also a commonly implicated nerve structure in many lower back and leg pain syndromes mostly due to structural compression concerns caused by a herniated intervertebral disc or osteoarthritic process.
This dialog focuses on L5 and how this nerve root is often the source of sciatica symptoms when it is compressed by a lumbar disc or bone pathology. We will investigate the symptoms of L5 pinched nerves and detail some diagnostic problems which typically occur.
Sciatica L5 Details
The L5 root leaves the spine at the lumbar 5 vertebral level. This area resides in the lower lumbar spine and is the most common region to experience degenerative disc disease and herniated discs, as well as general spinal degeneration, including lumbar osteoarthritis. This region is also the most common location for patients to suffer from vertebral misalignments, called spondylolisthesis.
L5 serves the motor and sensory needs of much of the lower body, in a pattern beginning on the rear outer aspect of the hip and tracing a diagonal line over the rear outer aspect of the thigh, to the outside of the knee and calf to the outer side and front of the shin to the top center of the foot, middle 3 toes and frontal bottom aspect of the foot under those same 3 middle toes. Most patients with L5 concerns have symptoms concentrated in the outer ankle, top of foot and big toe.
Problems with the L5 spinal nerve root can cause pain, tingling, numbness and/or weakness in any or all areas served, creating a usual sciatic nerve pain pattern.
Sciatica Lumbar 5 Causes
The L5 spinal nerve root meets with the L4, S1, S2 and S3 nerves to create the sciatic nerve. When a structure impinges on L5, it can occur within the central canal or in the neuroforaminal space. Since the cauda equina has already separated off the spinal cord at L5, any central or paracentral herniation which causes spinal stenosis may affect L5 within the central canal. Herniations might also block the neuroforaminal opening creating foraminal stenosis.
Arthritic bone spurs and debris can enact these same symptomatic profiles, as can ligamentous hypertrophy.
When vertebrae do not align properly, due to spondylolisthesis or some form of atypical spinal curvature, such as scoliosis or lordosis, pinched nerves can also occur within the central canal or more often, as they egress through the foraminal openings.
Sciatica L5 Factsheet
Pinched nerves can occur at L5, but will produce a definitive symptomatic pattern, especially when only L5 is compressed. This is why it is so crucial to seek diagnostic evaluation from a qualified neurologist, to be sure that the expression corresponds to the diagnosis.
Failure to correlate symptoms to L5 is one of the main reasons for misdiagnosis to occur and explains why so many patients can not find relief. This is logical, since if another causative process exists, then the treatments are not directed at the true symptomatic source.
In summary, please know that L5 is often involved in wide ranging pain syndromes, which may also involve many other nerve roots. These can be caused by cervical or thoracic spinal stenosis, large far lateral herniations in the lumbar spine, disease processes, regional neuralgias, piriformis syndrome and ischemia. Speak to your neurologist to make absolutely sure that L5 is the true and exclusive cause of sciatica before seeking any treatment.





