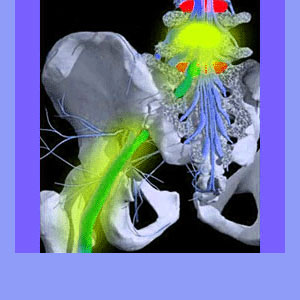
Sciatic nerve damage describes the unfortunate occurrence of structural injury to this largest of all bodily nerves. Nerve trauma can be minor or catastrophic and when it comes to the sciatic nerve, may involve the entire structure or just one or more of the spinal nerve roots which eventually form the main nerve itself.
Nerve damage is a much-abused diagnosis in the medical system, often used to explain why some patients never find lasting relief from sciatica. However, when the diagnosis is accurate, the consequences can be dire for the patient.
This dissertation examines the occurrence of neurological damage in the sciatic structure and its source nerve roots.
Sciatic Nerve Damage Injuries
The sciatic nerve itself can be damaged through traumatic injury. The most common sources of sciatic damage include car accidents, gunshot wounds and other serious puncturing traumas. Once damaged, the sciatic is likely to suffer lingering effects of the injury and may never regenerate 100%.
More commonly, one of the 5 spinal nerve roots which eventually join to form the sciatic nerve are damaged. This can occur due to back injury, such as a traumatic event, but is most common as an unwanted side effect of back surgery.
Surgical interventions are responsible for more spinal nerve damage than any other single cause. This can occur due to poor surgical technique, iatrogenic error, scar tissue formation or idiopathic causes.
Do I Have Nerve Damage?
What can be done about nerve damage? This is a common question that I receive every week from your letters and emails. Well, the answer may surprise you.
In cases of significant injury, sometimes damage is actual, structural and irreparable. The nerve may regenerate fully or partially, on its own, or it may not. Proper rehabilitation will certainly help increase the likelihood for better functionality.
Now for the surprising part: Most diagnosed cases of nerve damage do not exist at all or do not exist due to the reasons suspected. Some of these diagnoses are made after testing reveals diminished nerve function and the assumption is that damage has occurred. In the majority of these instances, there is no damage, just chronic and harmless, although often intolerably painful, ischemia which has caused functional impairment.
In some of the remainder of the cases, the mistaken diagnosis is sometimes made to cover up the poor curative results of a doctor who simply has nothing left to tell a patient:
“Doctor, you have tried to cure me with 9 different treatments.
Why do I still have pain?”
“I am sorry, Mr. Jones, you obviously have nerve damage.”
This is an excuse that makes me sick, and yes, it happens often.
Rarely will a doctor concede that their diagnosis may be flawed. No, that cannot possibly be. It must be nerve damage…
In other instances, the nerve damage is real, but not enacted by the original injury or degenerative process. Instead the damage may have been done exclusively by subsequent treatments, such as epidural injections or surgical intervention. Once again, this is virtually never disclosed to the patient.
Sciatic Nerve Damage Facts
Actual neurological damage is possible in many cases and may be just as bad as it sounds. However, in these circumstances, there is no doubt as to the findings, since the symptoms support the diagnostic theory 100%. In my experience, this rarely occurs.
Far more often, the diagnosis is made when a condition simply does not respond as a doctor hopes and some excuse is needed. This is the ugliest face of modern medicine and the nocebo effect of the mere inference of nerve damage upon a patient cannot be described.
I have worked with patients who were able to beat most of their physical pain in short order, but took years to dispel the undermining of their perceived health due to a literal curse cast upon them by a careless physician or chiropractor. They did not have nerve damage or any other lasting injury whatsoever. Some simply had ischemia and found permanent relief despite the claimed nerve damage. This is yet another example of how a mistaken diagnosis can almost cost a patient everything.





