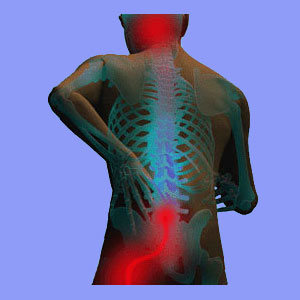
Sciatica from lordosis describes symptoms that are sourced due to a problem with the typical spinal curvature demonstrated in the lumbar region. Lordosis is defined as the normal front to back curvature of the cervical and lumbar spine, expressed with the open end of the curve facing the posterior of the anatomy. Lordotic curvatures are secondary developments and are formed after a person is born, at specific stages of infantile growth. This is unlike the kyphotic curvature of the upper back, which is congenital.
This exploratory essay will detail how abnormal lordotic curves can cause or contribute to sciatica, as well as how some atypical curvatures are unjustly blamed for causing pain.
Sciatica from Lordosis Definitions
Sciatica is a lower body neurological pain syndrome which always involves some form of spinal causation acting upon the lumbar nerve roots that eventually go on to form the body’s largest single nerve: the sciatic.
Pseudo-sciatica is an identical syndrome in its presentation and expression, but the source process is always a non-spinal source affecting the fully formed sciatic nerve itself.
Lordosis describes a normal and beneficial curvature found in the neck and lower back. This curve is not a side-to-side bend, but instead is a gentle front-to-back arc in the plane of the vertebral column. The curvature is conservative and is designed to better support weight, handle stresses and provide shock-absorption qualities to the spinal structures.
When the lordosis is increased or decreased, nerves can become trapped in misaligned or less-patent foraminal spaces, or inside a misaligned or narrowed central spinal canal, eliciting symptomatic expression. This is called lordotic sciatica.
Sciatica from Hyperlordosis
When the lumbar spine becomes increasingly curved, the condition is said to be hyperlordotic. This terminology simply means that the curvature is greater, when compared to the objective “normal”. Increased curvatures can decrease the patency of the central canal and the neuroforamen. This can lead to central spinal stenosis or foraminal stenosis. Both of these conditions can cause or contribute to painful sciatic nerve activity.
Lordosis can also affect or be affected by the surrounding spinal musculature, causing pain through a completely different musculoskeletal mechanism. In fact, muscular problems are one of the main instigators of lordotic changes. This is ironic, since these muscular contractions are often said to be the result of the curvature, instead of properly diagnosed as the underlying cause.
Sciatica from Hypolordosis
Hypolordosis is the exact opposite of hyperlordosis. In this scenario, the lumbar spine loses some or all of its natural curvature. In truly rare instances, the curvature might actually reverse direction completely and become kyphotic, rather than lordotic. This means that the open end of the curve now incorrectly faces the front of the body. Hypolordosis can lead to extreme pain, but this is not a given.
Just like with hyperlordosis, the potential effects are just the same. The foraminal openings and central canal can lose patency, possibly causing spinal stenosis or a pinched single nerve root.
Muscular problems can result, but these can also be the source process instead of a symptomatic expression, in much the same manner as in the hyperlordosis condition detailed above.
Sciatica Consequences
This article concentrates on lordosis in the lumbar spine. Changes in this area of curvature can certainly cause sciatica, when circumstances allow. However, there is another variety of lordotic change that can also cause sciatica-like symptoms.
Cervical spinal stenosis, enacted by lordotic alteration, can impinge on the spinal cord in the neck, potentially causing symptoms anywhere below the affected vertebral level. Many patients suffer symptoms in the legs, such as pain, weakness, numbness, the inability to stand or walk, as well as potential problems with the bowels, bladder or sexual organs. While this description does not embody the classic definition of sciatica, the expressions can be virtually identical. Patients are always warned to consider a cervical source, especially if the degeneration found in the lumbar spine is typical and not confirmed as being causative for the syndrome.
Elderly patients, and those with a history of neck problems or injury, should always keep this in mind, as cervical issues are often the actual causation of these types of pain conditions, while coincidental lumbar issues might mistakenly bear the blame.





