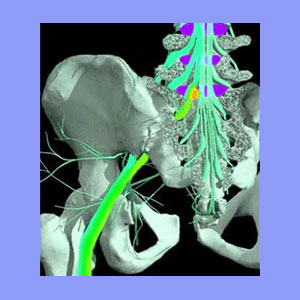
Sciatica from piriformis syndrome is a diagnosis often made in the absence of some structural spinal scapegoat on which to blame the pain. The piriformis muscles are located along the pathway traveled by the sciatic nerve. In cases of piriformis syndrome, the sciatic nerve is suspected to be compressed by the piriformis muscle due to injury or idiopathic causes.
Piriformis syndrome remains a hotly debated diagnosis, since many care providers do not subscribe to its existence at all, while others focus their entire practice around treating it.
This article will help to clear up the confusion of piriformis-related sciatica, by detailing how symptoms might occur in some patients, as well as providing an objective guide to preventing the common incidence of misdiagnosis.
Sciatica from Piriformis Syndrome
Piriformis syndrome is a very dubious diagnosis, since many cases are theorized to exist due to muscular injury. Most affected patients often do not remember hurting their piriformis, but the diagnosis is made nevertheless.
Injury can cause the piriformis muscle to spasm, just like any other muscular tissue on the body. However, this type of pain should resolve quickly, most commonly within hours or days, and is not at all likely to produce enduring sciatica symptoms.
Ischemia of the piriformis muscle and surrounding neurological tissues, including the sciatic nerve, can go on for months or even years. This type of piriformis-related pain is far more logical, but is typically not correctly diagnosed, since most oxygen deprivation syndromes are motivated by a psychosomatic process. Mindbody disorders are not acknowledged by most traditional healthcare practitioners, since they fall outside of their diagnostic comfort zones and often go against the accepted monetary standards of treatment. Translation: They do not make doctors any money.
Sciatica from Nerve Impingement
Some patients might demonstrate an anatomical predisposition to developing piriformis-related pain, due to a structural abnormality in which the sciatic nerve runs through the muscle, rather than below it. This irregularity is often found in patients with sciatica linked to piriformis syndrome. However, many people who have this abnormality do not have any pain and never suffer any unusual symptoms, making the structural link far from universal.
Some doctors who diagnose mindbody pain syndromes theorize that the subconscious mind is acutely aware of such anatomical abnormalities and often uses them to add credibility to psychoemotionally-induced pain conditions. This explanation seems to hold more creditability, since piriformis syndrome is one of the many conditions which can be cured using knowledge therapy, a completely psychological based treatment.
It is not unheard of for purely anatomical reasons to cause or contribute to piriformis sciatica either. These instances are just not common, compared to the number of patients misdiagnosed with piriformis syndrome. In these circumstances, muscle imbalances or deficits may affect the piriformis, causing it to tighten up on the sciatic nerve. It is also possible for some varieties of short leg syndrome to contribute to piriformis issues affecting the sciatic nerve.
Objective View on Sciatica from Piriformis Syndrome
Structural piriformis-related pain from a known injury should resolve in a matter of days or weeks at the very longest. If you have been diagnosed with piriformis syndrome, but have not found relief despite treatments and the passage of time, there is a good chance that the source of your pain has been incorrectly identified. In these cases, I recommend considering an alternative explanation which may involve the piriformis directly or indirectly. Ischemia can affect the piriformis, as can muscle issues and leg length concerns.
In all these scenarios, the piriformis muscle is not the cause of the sciatica expression unto itself, but is simply suffering the effects of a greater symptomatic process. Find and treat this process and the sciatica will disappear. Learn more about how the sciatic nerve can be influenced by the piriformis muscle on Piriformis-Pain.Com.




