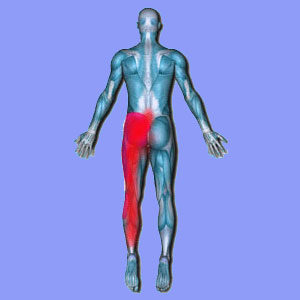
Sciatica in the back of the legs is the most common location for any type of lower body radiculopathy condition to strike. The majority of patients who are affected by sciatica endure symptoms in the buttocks, back of the thighs and back of the calves, although symptoms are generally possible anywhere in the lower body region.
When pain is blamed on a structural spinal issue, such as a herniated disc, it is truly crucial to describe exactly where the symptoms occur, since this can help support or rule out a particular diagnostic theory. Remember, every nerve root in the lower back innervates a particular region of the lower body anatomy. If the location of the symptoms does not match the causative condition, then it is a safe bet that the working diagnostic theory is wrong. This fact is sadly rarely considered by some non-neurologist care providers.
This dialog focuses on sciatica expressions in the rear of one or both legs.
Sciatica in the Back of the Legs Conundrum
Sciatica which occurs in the rear of the legs can take the form of pain, tingling, numbness or weakness. Often, patients have a variable symptomatic expression which may change randomly or in a set pattern.
Being that sciatica involves nerve tissue, locating exactly where the symptoms occur can be difficult, as many patients suffer shooting or radiating pain which affects a regional area, rather than a specific spot.
Other common patient complaints involve feelings of heaviness in the rear of the legs, occasions of sharp crackling pain or a feeling of actual burning inside the leg. I have suffered many of these myself and know how brutal they can be to endure.
Sciatica Solutions
Regardless of where your sciatica occurs, my advice is always the same: In order to find relief, you must know what is actually causing your pain and then you must treat it appropriately.
Sciatica is known to be a fierce and treatment-defiant condition, but only because the suspected source of pain is often misidentified, leading to treatment which targets a mistaken causation. How can a treatment work if it is not directed at the actual source process which is responsible for the pain?
Therefore, I advise every patient to concentrate on their diagnosis and do whatever you can to prove or disprove a diagnostic theory before seeking treatment. This may seem difficult, but it is really just a matter of learning many of the facts about sciatica and comparing the actual symptoms to the clinical expectations. Your spinal neurologist will prove very useful in this regard.
Managing Sciatica in the Back of the Legs
Pseudo-sciatica in the backs of the legs is also a common diagnostic theory, usually being linked to piriformis syndrome or extended periods of sitting.
In many instances, the symptoms exist solely in the backs and the legs and may seem to come from a structural issue. In a few cases, this theory is actually correct, but in other circumstances, the diagnosis is wrong, once again leading to unsuccessful therapy to treat the piriformis muscle or sacroiliac joint.
In my experience, a great number of sciatica from piriformis syndrome cases are ischemia conditions which have been only partially diagnosed correctly by care providers who do not even understand how the oxygen deprivation process works. They merely see its effects on the piriformis and deem this muscle to be the source of pain, rather than just one of the results of a greater and more widespread condition. If this is your reality, take care and consideration before acquiescing to any drastic or surgical treatment modality.
Of course, in cases where a structural diagnosis can definitively be proven, and symptoms correlate by expression and location, medical intervention may be needed. The proper therapy will depend on whether central spinal stenosis, foraminal stenosis or a non-spinal concern is judged to be the cause, as well as other patient-specific criteria. Please see the sciatica treatment resource section for detailed information.
Sciatica > What is Sciatica > Sciatica in the Back of the Legs





