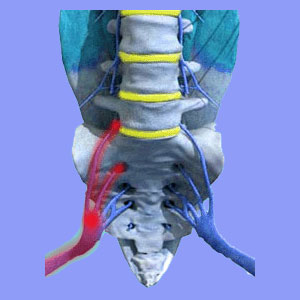
Sciatica neuropathy is another long winded term for non-specific nerve pain which involves the sciatic nerve, the nerve roots which create the sciatica nerve or any of its peripheral branches. Neuropathy is a diagnostic description used for nerve pain anywhere in the body, as opposed to mechanical pain or other types of anatomically-motivated suffering.
Nerve symptoms can be notoriously difficult to accurately diagnose and the incidence of misdiagnosis of sciatica patients has reached epidemic proportions in the back and neck pain sector. Even the best neurologists will explain that accurate diagnosis of nerve conditions can be hit or miss. It is no surprise that many chronic patients never do find real or lasting resolution of symptoms.
Sciatica Neuropathy Variations
Sciatica, unto itself, is a very non-specific diagnostic theory. It simply pronounces that the sciatic nerve is theorized to be involved in the painful symptomatic expression. Neuropathy is no better, since it also simply mentions that nerves are the main source of suspected symptoms, rather than bone, muscle, ligament or tendon.
Sciatica and neuropathy together suggest an even more vague diagnostic analysis, since it is not clear if the sciatic itself is the source, or some part of the peripheral nervous system which forms or branches off the sciatic.
Regardless of all this terminology, the curative statistics offered by most treatments for any type of neuropathy syndromes are usually quite poor. This always reminds me that the diagnosis itself may be wrong, so the treatments prescribed may not be targeting the correct root cause of the nerve pain. Of course, this is assuming that any definitive diagnosis is rendered at all.
Sciatica Neuralgia Facts
Most sciatica conditions are theorized to exist due to causative problems in the spinal nerve roots prior to formation of the actual sciatic structure. Most typically, these concerns include intervertebral disc issues, such as herniations, and vertebral issues, such as spinal osteoarthritic changes. In other circumstances, spinal curvature abnormalities or vertebral misalignment concerns are suspected of compressing the affected nerve roots. While all these conclusions are certainly possible, many are incorrectly identified as the source of pain, despite structural changes which may truly exist, but are purely inconsequential and coincidental to the symptoms expressed. When the diagnostic theory is right, then therapy is typically successful.
In other cases, the fully formed sciatic nerve itself is thought to be compressed, usually by the piriformis muscle. This diagnosis can also truly take place, but sometimes not for the reasons usually suspected, which include localized injury or muscle imbalance.
In many cases, piriformis syndrome is a direct result of ongoing muscular ischemia. This is far more logical, since oxygen deprivation of the piriformis will cause the muscle to clamp down on the sciatic nerve, eliciting potentially painful and disturbing neurological expressions.
Sciatica Neuropathy Guide
Neuropathy and sciatica are diagnostic cop-outs in most cases, regardless of where the symptoms occur. This is because both are actually symptom sets and not self-contained causative conditions. These conclusions almost always pre-suppose injury or degeneration of some structural part of the spine, although research statistics clearly show these same structural issues to be innocent in most cases. While there is no universal way to prevent misdiagnosis of sciatic nerve pain, there are some ways to minimize the risk:
Always get more than one opinion from more than one type of doctor. Be sure to include at least one spinal neurologist.
Always do independent research to learn everything about the working diagnostic theory.
Always compare the expected symptoms matching the diagnosis to the actual symptomatic expression and look carefully for discrepancies. This is the most telling factor indicating misdiagnosis in my experience.





