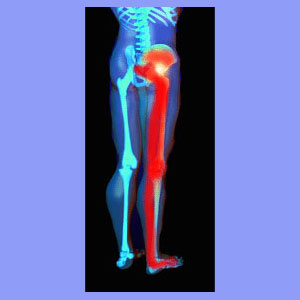
A pinched sciatic nerve is actually an anatomical impossibility if the suspected cause is supposed to exist in the spine. This is because the sciatic nerve does not connect directly to the spine at all. The sciatic nerve is made up of 5 pairs of spinal nerve roots which exit the spinal cord at vertebral levels L4 through S3. It is generally one of these spinal nerve roots which is actually affected when the diagnosis of a compressed sciatic nerve is made.
However, sciatic compression can occur further down in the anatomy, enacted by muscular constriction or localized trauma, such as a crushing or penetrating injury. This essay will clarify the diagnosis of sciatic nerve compression and enlighten patients on the anatomical facts of the condition.
Pinched Sciatic Nerve Condition
In cases of spinally-enacted sciatica, the nerve roots will be the tissues affected by compression, not the sciatic nerve itself.
Spinal causes for a pinched nerve root can include herniated discs, osteoarthritis or spondylolisthesis, as well as atypical side to side or front to back curvature concerns. These structural irregularities are often targeted as the cause of a pinched nerve root, but can not logically be implicated in pinching the sciatic nerve directly.
However, if one of the spinal nerve roots which comprise the sciatic nerve is affected by constriction, radicular pain might result and can influence the function of the sciatic nerve in transmitting nerve messages to the lower anatomy. Just remember that pinched nerves are diagnosed far more often than they actually occur and represent one of the most common forms of misdiagnosed sciatica.
Actual Compressed Sciatic Nerve
Piriformis syndrome is a condition which might actually compress the sciatic nerve itself, as the nerve passes through the greater sciatic foramen while leaving the pelvis. In about 15% of the population, the sciatic nerve passes directly through the piriformis muscle, rather than underneath it.
In the controversial piriformis syndrome diagnosis, this muscle is theorized to constrict the sciatic nerve, usually due to some form of trauma, although the source or nature of that trauma can not usually be identified.
Although this condition does truly exist, a far more plausible and logical explanation for the pain might be ischemia of the piriformis muscle. This theory certainly logically rationalizes why many patients have muscular spasms in the piriformis which can not be explained due to any other factor.
Pinched Sciatic Nerve Conclusions
Remember basic anatomy when dealing with any nerve compression issue. Even assuming that one or more of the spinal nerve roots are being impinged upon by some structural causation, such as a herniated disc, studies have shown 2 factors which make chronic sciatica seem unlikely:
1. Very few spinal conditions cause long-term pain. Most herniated discs resolve on their own and most minor osteoarthritic processes are not inherently painful.
2. In cases of verified continued nerve compression, the result is complete numbness, not pain. Sustained compression of a spinal nerve root will cause that root to stop signaling altogether. Lasting pain seems like an anatomical impossibility in these instances.
Learn the facts about sciatica and you will better understand how nerve compression can occur in various locations of the anatomy. Do not allow your physician to tell you that you have a herniated disc pinching your sciatic nerve. Tell them to study their anatomy lessons and stop treating you like an idiot. Insist on being told the facts the way they truly occur, instead of some watered-down version provided to a child. If your doctors can not treat you with the dignity and honesty you deserve, then it is certainly time to consider replacing them with a physician who can and will.





