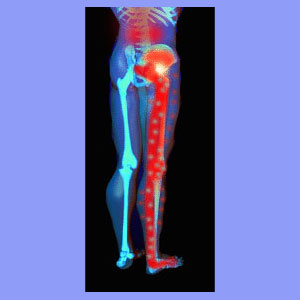
Back and foot pain is generally theorized to be caused by compression of the nerve roots located between the lumbar vertebrae L4, L5 and S1. These spinal nerves control the muscles and sensory perceptions of the feet and are often implicated in foot pain and related neurological syndromes, especially in the presence of lower back pain. That being said, it is crucial to understand that other processes can also cause similar symptomatic expressions.
This article will detail all the usual sources of back pain and foot pain which may be related, as well as coincidental to one another.
Back and Foot Pain Causes
Most often, there is some spinal abnormality blamed for causing manual compression of one of the lumbar or sacral nerve roots as it leaves the spinal column. Herniated discs are the most common causative condition, but many patients might also be diagnosed with foraminal stenosis due to degenerative disc disease and/or spinal osteoarthritis. Sometimes, these same structural conditions can affect the entire cauda equina directly, causing lumbar spinal stenosis. While all these scenarios are possible and do occur in some patients, they are often misdiagnosed as the actual cause of pain in many individuals.
Most patients do not know that central spinal stenosis in the upper back or neck can also enact sciatica back and foot pain, among numerous other dire neurological expressions.
Piriformis compression of the actual sciatic nerve occurs long after the nerve roots have left the spine, but can also create buttocks, leg or foot pain unilaterally or bilaterally.
Systemic and disease processes, such as various forms of neuropathy can create foot pain, as well as back pain. Oxygen deprivation of the spinal nerve roots is a common source of these same terrible symptoms.
Back and Foot Symptoms
Regardless of the actual causation of the problem, most patients suffer a host of uncomfortable symptoms in the back, legs and feet. Sciatica pain is very common, especially in the back and upper legs. Tingling, weakness and numbness are especially common in the thighs, lower legs and feet.
Generally, for foot complaints, the L4, L5 and S1 nerve roots are implicated, depending on the exact area affected. The more diverse the symptomology of a sciatica pain syndrome is, the less the chance of it coming from a single spinal source. Additionally, the more a pain syndrome changes in its symptomatic expression, location or intensity, the less the chance of it originating from a spinal causation at all. The exception to these rules is central stenosis, which is known to enact highly variable and patient-specific symptoms.
Unilateral sciatica is statistically more likely to be correctly identified as coming from a spinal nerve compression syndrome than bilateral sciatica.
Back and Foot Pain Conclusions
I originally experienced virtually no foot pain in relation to my long standing battle with lower back pain, but have endured a tremendous amount of tingling and numbness in my feet during acute attacks.
I used to get shooting pins and needles sensations across the bottom of my feet often and would also sometimes experience cramping and spasms in my toes and arches. This was all blamed on my lumbar degenerative disc disease and 2 herniated discs at L4/L5 and L5/S1.
I tried everything to relieve my back and leg pain, as well as my neurological foot symptoms, to no avail. At this stage, more than 25 year later, I have more pain in my back and neck than ever before, in terms of the diversity of locations. However, it is not usually debilitating. I do get far more foot pain and also suffer recurrent spasms, especially when flexing my toes or elevating my legs, such as when trying to rest in bed.
Before wrapping up this article on back and feet symptoms, I need to stress the obvious, but not always considered, fact that many symptoms might be coincidental to one another. What I mean is that a person might have foot pain due to a localized source and may also have unrelated back pain.
Heel spurs, tendonitis, plantar fasciitis and metatarsalgia are all common foot pain diagnoses which may be completely independent of any sciatic nerve symptoms. Remember, just because there are 2 sets of symptoms, in the back and in the feet, does not mean they are inherently related.
In order to better the chances of confirming or disproving the relationship between the 2 expressions, be sure to consult with a qualified neurologist for nerve conduction testing and symptomatic correlation.





