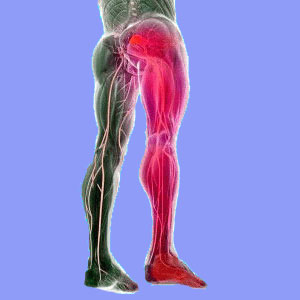
Pseudo-sciatica is a diagnostic term sometimes used to describe sciatic nerve symptoms which are not caused by the typical spinal sources. The term pseudo means false or not real. However, it is a very bad choice of words for this diagnosis for multiple reasons, since the pain is indeed very real and a great number of all sciatica pain syndromes should actually be considered pseudo.
This essay will focus on the nonspinal sources of sciatica symptoms, including a variety of structural and nonstructural causative conditions.
Pseudo-Sciatica Versus Sciatica
Sciatica is considered a lower back and leg pain syndrome caused by some structural abnormality in the spine. The reason for the symptoms is almost always thought to be the result of nerve compression, either of individual spinal nerve roots or the actual spinal cord or cauda equina itself. The typical conditions blamed for creating this nerve compression include:
A lumbar herniated disc can press on a nerve root through the process of lateral or foraminal stenosis or may impinge on the actual spinal cord or cauda equina through the process of spinal stenosis.
Osteoarthritis might cause osteophyte growth which compresses a nerve root or reduces the patency of the central canal, causing spinal stenosis.
Spondylolisthesis can cause the central or foraminal canals to line up incorrectly, possibly pinching a nerve.
To simplify, pseudo-sciatic nerve symptoms mimic the usual pain profiles of true sciatica, but are diagnosed as being caused by a nonspinal source.
Causes of Non-Spinal Sciatica
There are 2 conditions currently blamed for the majority of pseudo sciatic nerve symptoms. In some cases, these diagnoses might logically explain symptoms, while in others, the diagnostic theory is illogical and often far fetched:
Piriformis syndrome is a condition in which the powerful piriformis muscle is thought to constrict the actual sciatic nerve, deep inside the pelvis. While this condition can exist, it is quite rare and is diagnosed far more commonly than it actually occurs.
Sacroiliac joint pain is often blamed for ongoing pseudo sciatic nerve pain. Most SI joint pain syndromes are localized and will not provide the types of far ranging symptoms often mistaken for true sciatica. Sciatica from the sacroiliac joint is possible, but rarely affects the same large area as true sciatica.
Ischemia can be the source process for pseudo sciatic nerve symptoms, but can also cause real sciatica, as well. Many spinal sciatica complaints have been grossly misdiagnosed, which explains the dismal results of most treatments. Ischemia does not enact any actual pinched nerves, but can deprive any of the neurological tissues of necessary oxygen, severely limiting their capacity to function. This can occur to a single nerve root in the spine, multiple nerve roots or may even affect the entire cauda equina structure, eliciting a diversity of terrible symptoms. Similarly, ischemia can also affect the sciatic nerve itself, far below the actual spinal nerve roots.
Pseudo-Sciatica Realities
Since many suspected spinally-induced sciatica syndromes are actually misdiagnosed and caused by simple ischemia, localized nerve dysfunction, muscular issues or disease processes, then the word pseudo is really quite redundant. In fact, most sciatic nerve pain is pseudo, if you accept that definition of a non-spinal source.
Personally, I couldn’t care less what you call it. Sciatica is a misery to endure and virtually impossible to cure, as long as you embrace those tired old medical myths about why it exists or seek treatment from a care provider who does.
Do your own research and learn the facts about sciatica for yourself. You will discover that the symptoms do not often correlate to the theorized diagnosis, which really helps to explain why all the treatments you have tried have failed. Get off this vicious cycle before you waste more time and money seeking contraindicated and necessary care.
The lesson to be learned here is that just because a lumbar spinal abnormality exists, does not mean it is the cause of your sciatica. In most cases, mild to moderate disc and bone irregularities are innocent of causing any symptoms at all.
Meanwhile, a non-spinal source could be the actual causation all along. Never forget to consider this possibility in order to improve your chances for finding a cure. Speaking of cures, our proprietary Cure Back Pain Forever Program works wonders for virtually all cases of pseudo-sciatica. This is why the program has enjoyed such positive reviews from doctors and healthcare organizations.





