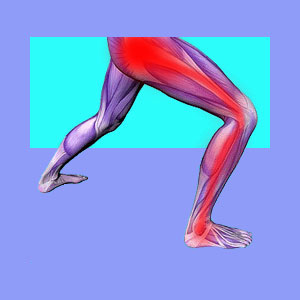
Muscular causes of sciatica can perfectly mimic spinal sources in their expression. Some pseudo-sciatica syndromes are created by muscular issues, perpetuated by muscular concerns, or are simply expressed in the muscles of the buttocks, legs and/or feet.
True sciatica will always be traced to a spinal cause in the lumbar region. In order to fit the medical definition of sciatica, the nerve roots at L4, L5, S1, S2 or S3 need to be affected within the spinal anatomy. Therefore, many sciatica-like syndromes should be classified as pseudo-sciatica, meaning that they are exact clones of true spinally-induced sciatica but are not caused by compression or chemical irritation of the usual typical lumbosacral neurological tissues.
This patient guide examines many of the possible muscular origins for sciatica symptoms. We will focus on discussing piriformis syndrome, regional ischemia and localized causes of buttocks, leg and/or foot pain, as well as other expressions, such as paresthesia and weakness.
Muscular Causes of Sciatica Due to Injury
Many patients suffer acute, recurrent or chronic injury to one or more of the muscles, tendons or ligaments in the buttocks, legs or feet. Since all these soft tissues work together to allow us a complete range of motion, it is common that pain can affect a relatively large region, even when only one soft tissue structure has been compromised.
The most common regions for muscular injury and subsequent pseudo-sciatica expressions are the hip and the knees, both of which can create pain that might mirror sciatica in many ways, including the generation of pain and weakness. The ankle and foot are less common sites, but can certainly occur and might also source seeming sciatica symptoms, even without neurological involvement.
Some patients will suffer a combination of muscular injury and related compression of the fully formed sciatic nerve or one of its peripheral branches. Traumatized muscles might spasm, possibly compressing these nerve tissues inside the buttocks or leg, causing a combination of injury-related pain and sciatic nerve impingement that can affect much of the remainder of the lower leg or foot. This is one theory used to explain piriformis syndrome, which is detailed below.
Regional soft tissue injury can occur from many scenarios, including sports traumas, car accidents, falls or any event that damages the buttocks, leg or foot. Acute traumas will usually not leave residual symptoms and should heal completely in a defined timeframe. Recurrent and chronic injury, such as that suffered by some athletes, might create long-lasting or permanent symptoms in affected regions of the lower anatomy.
Muscular Causes of Sciatica Caused by the Piriformis
Piriformis syndrome is a diagnosis wherein the fully formed sciatic nerve is theorized to be compressed by the piriformis muscle. This small, powerful muscle in located in the buttocks, near the area of the hip. In most people, the sciatic nerve passes underneath this muscle as it traverses the path down the leg. In some people, the nerve actually passes through the muscle, since they demonstrate an anomaly with the natural design of the piriformis tissue. It is no surprise that the piriformis syndrome diagnosis is far more common in people who demonstrate this atypical anatomical profile, but this is not an absolute rule by any means. Many people have pseudo-sciatica blamed on piriformis nerve compression despite not being affected by this abnormal developmental trait, while others do indeed demonstrate the nerve-through-muscle trait, but suffer no symptoms.
Since the entire sciatic nerve is theorized to be compressed high in the buttocks, effects can be wide-ranging and might affect the local area of compression, as well as the entire leg or foot unilaterally or bilaterally. Symptoms might be consistent or might change regularly, as is common with all manner of sciatica and pseudo-sciatica syndromes.
Piriformis syndrome has become an ever-more controversial diagnostic theory, since many physicians see no proof of any compressive process being applied to the sciatic nerve in most suspected cases. In essence, the anatomy is deemed to be normal and non-pathological, even when the nerve passes through the muscle. This is why detailed location-specific nerve conduction testing is recommended to patients who receive a diagnosis of piriformis-related symptoms.
Muscular Causes of Sciatica Caused by Oxygen Deprivation
Oxygen deprivation can occur for many reasons, including circulatory problems, blood cell problems or mindbody causes. Since the first 2 possibilities can be easily diagnosed with various basic tests, we will focus our spotlight in this section on the mindbody variant of ischemia.
Although originating in the subconscious mind, ischemia can target muscular or neurological tissues in a regional area. One of the more common targets of these psychogenic pain conditions is the sciatic nerve and its surrounding anatomy.
Some patients might experience ischemia of the muscles, ligaments or tendons in the buttocks, legs or feet. In some instances, this oxygen reduction can cause cramping and spasming of the tissue, which may in turn compress neurological tissues. In this regard, the piriformis syndrome diagnosis detailed above makes much more sense. In other circumstances, ischemia might be directed at the sciatic nerve itself, the nerve roots that create it, or the peripheral branches of the nerve. In most patients, it seems that both muscular and nerve tissue is often affected simultaneously.
Since ischemia is such a variable process that leaves no easily discovered clinical evidence, it is rarely diagnosed as the actual cause of pain, tingling, numbness or weakness. This is particularly true for mindbody versions of the condition, which are often diagnosed as tension myoneural syndrome by the few trained specialists who are qualified to recognize the disorder for what it truly is.
To learn more about any of these possible muscular causes of sciatica pain, please talk to your doctor. Alternatively, for a complete and objective look at these, and other potential sciatica causes, continue studying and enjoying this website, since we cover the topic of lower back and leg pain in unrivaled detail.





